What is Hypertrophic Cardiomyopathy?
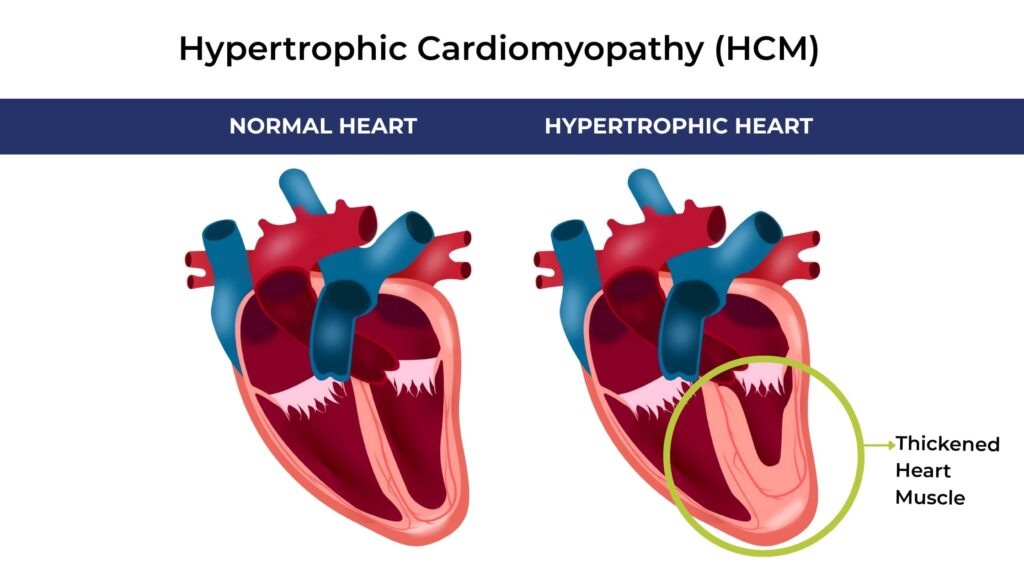
Hypertrophic cardiomyopathy (HCM) is a genetic heart condition in which the heart muscle becomes abnormally thick. This thickening is caused by a mutation in one of the genes that controls heart muscle structure and function.
The abnormal heart thickening typically develops in the teenage years and then usually remains stable throughout life. However, the extra muscle can interfere with the heart’s ability to pump blood efficiently and may increase the risk of heart rhythm abnormalities (arrhythmias).
In some cases, the thickened muscle partially blocks blood flow as it leaves the heart. This form of the condition is known as hypertrophic obstructive cardiomyopathy (HOCM).
HCM affects each person differently. Some individuals have no symptoms, while others may experience:
- shortness of breath,
- chest pain,
- fatigue,
- dizziness, or
- fainting.
Although HCM is a lifelong condition and cannot be cured, many effective treatments are available to manage symptoms, reduce complications, and support a full, active life.
Because HCM requires ongoing monitoring and specialized expertise, long-term care with an experienced cardiology team is essential.
Patient education resource: The American College of Cardiology provides trusted, patient-friendly information through its CardioSmart program.
Hypertrophic Cardiomyopathy Care at VCS
Virginia Cardiovascular Specialists (VCS) provides comprehensive, specialized care for patients with hypertrophic cardiomyopathy across our practice.
Each VCS location includes one or more cardiologists with specific expertise in HCM, ensuring you receive knowledgeable, personalized care close to home. When advanced testing or procedures are needed, your care team can seamlessly coordinate access to specialized services available throughout the VCS network.
Our HCM services include:
- Advanced cardiac imaging, including cardiac MRI
- Cardiac electrophysiology evaluation for arrhythmia risk
- Prescription therapy, including mavacamten when appropriate
- Alcohol septal ablation for select patients with obstructive disease
Above all, VCS emphasizes shared decision-making. We partner with you to understand your goals, explain your options clearly, and guide lifelong care for both you and your family.
Initial Evaluation and Follow-Up Care at VCS
Care for hypertrophic cardiomyopathy at VCS follows a standardized, evidence-based protocol grounded in the latest national guidelines and clinical research. These protocols are regularly updated as new data and therapies emerge.
Initial Evaluation May Include:
- Consultation with an HCM-experienced cardiologist for education and care management planning
- Electrocardiogram (EKG)
- Comprehensive echocardiogram
- Wearable cardiac monitoring (1–14 days, based on clinical needs)
- Cardiac MRI
- Stress echocardiogram to assess for outflow tract obstruction, when indicated
- Review of family history and discussion of genetic testing
- Cardiac electrophysiology consultation, if needed
Ongoing Follow-Up Care Typically Includes:
- Annual office visits (or more frequent visits if needed), with EKG
- Echocardiogram every 1–2 years, or sooner if symptoms change
- Periodic wearable cardiac monitoring for 1-14 days, every 1–2 years, based on risk
- Cardiac MRI every 3–5 years for select patients under age 60 without an implanted defibrillator
- Stress echo to look for outflow tract obstruction may be performed based on symptoms
- Follow-up on status of family screening and genetic testing
This structured approach allows for proactive monitoring, early intervention, and continuity of care over time.
Hypertrophic Cardiomyopathy (HCM) Program Leadership
HCM Program Coordinator: Dr. David Gilligan
Echocardiography Program Director: Dr. David Soma
Alcohol Septal Ablation: Dr. Matthew Chung